Discharge from a nipple in a woman who is not pregnant or breast feeding is an abnormal symptom. A study showed that about 3-9% of patients reporting to a breast clinic with a breast symptom presented with a nipple discharge. Nipple discharge may be caused by many underlying conditions in a non-pregnant and non-lactating woman. When discharge is milky and occurs in both breasts, the underlying cause may be abnormal levels of a hormone that stimulates the milk ducts. A blood test is needed to confirm this. If abnormal levels of prolactin are found, MRI imaging of the brain is needed, to exclude a small tumor of the pituitary gland that is responsible for the elevated levels of prolactin. Milky, white or greenish colored discharge from the nipple are generally considered physiologic and benign and in most cases, are caused by benign breast conditions such as fibrocystic changes or inflammation of the ducts.
Please schedule a consultation with Dr. Shetty if you experience any abnormal breast symptoms to learn how breast imaging can help you.
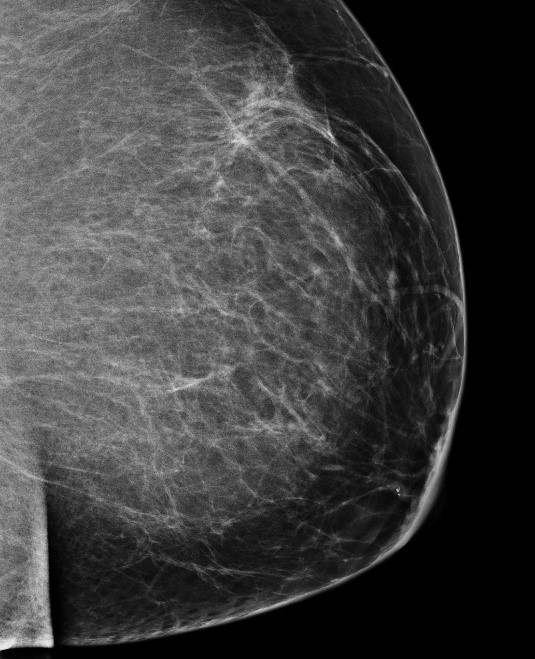
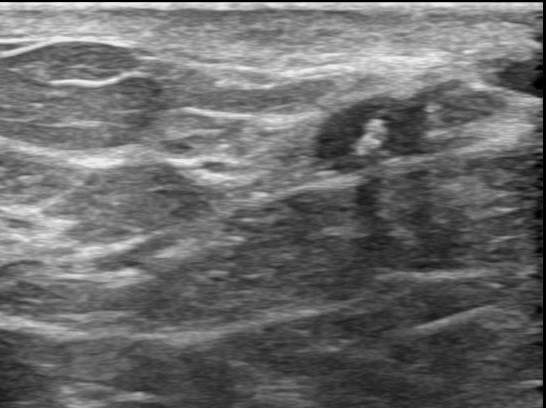
Nipple discharge is regarded as pathological if blood stained, serosanguinous, serous or clear. In some women, the discharge may result from a benign growth in the duct called a papilloma and in others caused by a cancer growing inside a duct. It has been reported that in about 5-12% of women with a bloody one breast nipple discharge there is an underlying cancer, such patients often have an associated lump. A discharge from the nipple of one breast that is spontaneous and blood stained should be therefore prompt a physician consultation. Investigation of this symptom is triple assessment: Clinical examination to look for a palpable lump, cytological testing of the discharge fluid and diagnostic imaging with a mammogram and breast ultrasound (Image 1 and 2).
Image 1. Left breast mammogram showing a small papilloma underneath the nipple in a patient with bloody nipple discharge
Image 2: Ultrasound showing the same tumor
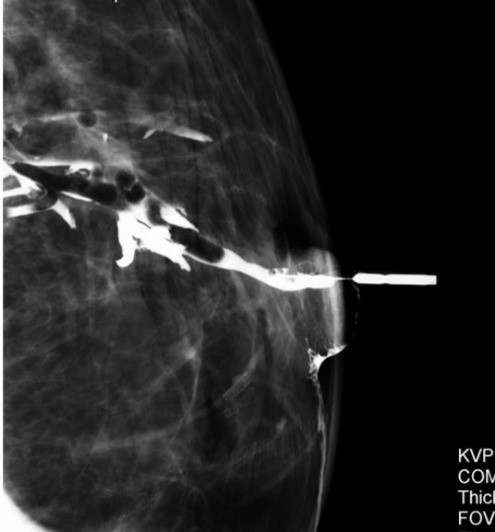
Cytology when positive is helpful, when negative is not reliable to exclude an underlying breast cancer. Imaging evaluation is needed to identify the underlying cause of the nipple discharge. When these tests do not identify a specific cause, additional evaluation may be needed such as a ductogram where a radiopaque dye is introduced into the duct with the abnormal discharge, to precisely identify and localize tumors in the duct (Image 3).
Image 3: A ductogram shows tumor inside the duct outlined by the white dye in a patient with bloody nipple discharge that was proven to be a non cancerous papilloma at surgery
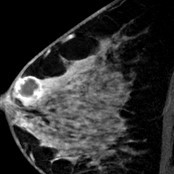
Ductoscopy is an additional technique to directly visualize and examine the ducts for tumors, this is however a specialized test that is not widely available. Breast MRI is an alternate imaging tool to Ductography to identify ductal tumors or underlying cancers causing abnormal discharge from the nipple (Image 4).
Image 4: A breast MRI image shows a tumor in the breast in a patient with nipple discharge that was proven to be a breast cancer at biopsy
If an intraductal tumor is identified on an imaging study a minimally invasive needle biopsy is performed under imaging guidance under local anesthesia. This is a quick and safe outpatient procedure. Most papilloma’s in the breast require surgical excision since they may be associated with early stage or low-grade cancers. For those women with persistent blood-stained discharge and no identifiable cause on imaging studies, surgical excision of the subareolar ducts is a surgical option, generally for women over the age of 40 years who do not intend to breast feed, for younger women less aggressive surgical option of resection of the just the symptomatic duct is performed.
In summary nipple discharge is a breast symptom that requires a physician consultation and possible imaging evaluation. When this symptom is spontaneous, bloody and affecting one breast, there is a small but significant association with a papilloma or breast cancer.
Resources:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1964556/
https://www.cancer.gov/types/breast/breast-changes