The burden…The American Cancer Society estimates for ovarian cancer in the United States for 2018 22,240 women will receive a new diagnosis of ovarian cancer. About 14,070 women will die from ovarian cancer. Compared to breast cancer the death rate is significantly higher because cancers are diagnosed at an advanced stage due to lack of a screening test like mammography. Ovarian cancer ranks fifth in cancer deaths among women, accounting for more deaths than any other cancer of the female reproductive system. This cancer mainly develops in older women. About half of the women who are diagnosed with ovarian cancer are 63 years or older. There are less aggressive types of ovarian cancer that tend to affect younger women. These include germ cell tumors, stromal tumors and borderline ovarian tumors of the ovary. Women with a family history of ovarian cancer have an increased risk of developing ovarian cancer. The lifetime ovarian cancer risk for women with a BRCA1 mutation is estimated to be between 35% and 70%. This means that if 100 women had a BRCA1 mutation, between 35 and 70 of them would get ovarian cancer. For women with BRCA2 mutations the risk has been estimated to be between 10% and 30% by age 70.
To learn more about receiving a pelvic ultrasound in Houston with the expertise of Dr. Shetty, contact the Pink Door Imaging today.
The symptoms associated with Ovarian cancer
Ovarian cancer used to be referred to as the silent killer because symptoms were thought not to present until late stages. Evidence now indicates that women diagnosed as having ovarian cancer, including those with early-stage disease, have symptoms that predate diagnosis by 3–36 months.
• Feeling full after eating only a few bites or loss of appetite
• Diarrhea, constipation, bowel or rectum feels full
• Change in bowel habits, constant urge to have a bowel movement, painful or burning bowel movements, pain, painful defecation
• Bloating, distension of abdomen, clothes around the waist feel too tight, feel an abdominal mass
• Weight loss not because of dieting
• Nausea, vomiting, heartburn, gas, burping, indigestion
• Increased urinary frequency, need to urinate urgently
• pressure on the bladder, leaking urine, burning sensation when urinating, need to urinate but unable to do so, unable to empty bladder completely, feeling full after urinating
• Vaginal discharge, bleeding, spotting, deep pain on intercourse
• Discomfort or pain in abdomen, pelvic region, or lower back
The Diagnosis
Ovarian cancer remains the most common cause of gynecological cancer death. Whereas < 5% of women survive the disease for 5 years if diagnosed at the most advanced stage (IV), when diagnosed early (at stage 1) 90% survive. Transvaginal ultrasound is an accurate test to assess the ovaries. Ovarian cancer has characteristic appearance on ultrasound. Typically, when a tumor is found the Radiologist assesses the morphologic features of the tumor, a Doppler examination is an integral part of the pelvic ultrasound assessment of the ovaries. Doppler evaluation identifies the pattern and type of blood supply to the tumor. It can provide indication whether the tumor is cancerous or not. The key is finding the cancer when small. However, since Pelvic ultrasound is not offered as a screening test, ovarian cancer is seldom found when small (Figure 1) and when diagnosed by a pelvic ultrasound is often large (Figure 2) leading to an unacceptable high mortality rate because of the advanced stage of disease. In some cases, pelvic ultrasound may be inconclusive and additional testing with a pelvic MRI may be needed. Having a pelvic ultrasound in Houston with skilled sonography technologists and a Radiologist with experience and expertise in Gynecological pathology is important for an accurate diagnosis. There can be an overlap in the appearance of the ovarian cancer particularly when small, with non-cancerous and physiologic abnormalities of the ovaries. Lack of experience or an understanding of these mimics can lead to unnecessary surgeries.
Should we be screening women for ovarian cancer with annual Pelvic Ultrasound in Houston?
To be applicable as an effective screening test, we need to have a test that is safe, accurate and with a low false positive rate and false negative rate. Several trials have been undertaken to determine the value of transvaginal pelvic ultrasound in screening for ovarian cancer by itself or in combination with a blood test that is often used in the diagnosis of ovarian cancer, the CA-125. Use of transvaginal ultrasound alone for routine screening for ovarian cancer has not been shown to be cost effective and is also limited by a high false positive rate. So, investigators have studied the benefit of performing ultrasound on women who are at an elevated risk based on symptoms, elevated CA-125 or a combination thereof.
Recent studies have shown benefit of using transvaginal pelvic ultrasound in women with an abnormal CA-125 in early detection. Pelvic Ultrasound with endovaginal ultrasound done annually also may benefit women with a family history of ovarian or gynecological cancer.
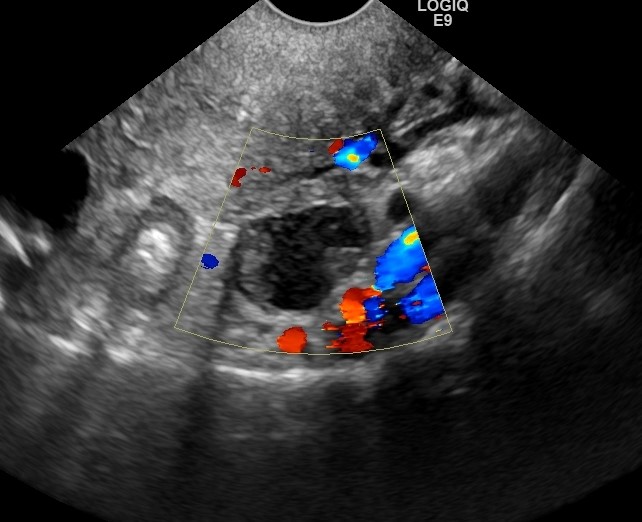
Figure 1. Endovaginal Ultrasound showed a small tumor in the ovary (arrow) that was considered suspicious for cancer, at surgery a small ovarian cancer was discovered.
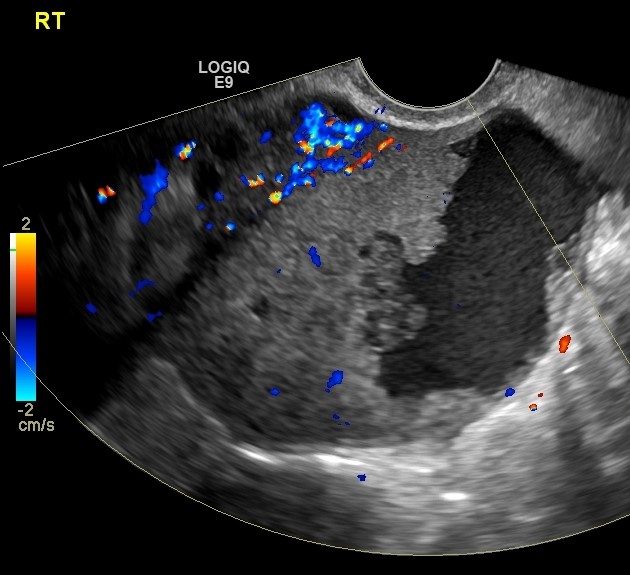
Figure 2. Pelvic Ultrasound shows a large ovarian cancer in a woman who presented with symptoms of abdominal bloating and a mass on Physical examination
Resources:
• https://www.cancer.gov/types/ovarian
• Adnexal Masses: Role of Supplemental Imaging With Magnetic Resonance Imaging. Shetty MK. Semin Ultrasound CT MR. 2015 Aug
• Ovarian cancer screening and mortality in the UK Collaborative Trial of Ovarian Cancer Screening (UKCTOCS): a randomized controlled trial. Jacobs, Menon. Lancet 2016; 387: 945–56
• https://www.cancer.org/cancer/ovarian-cancer/about.html
• https://www.ncbi.nlm.nih.gov/pubmed/22257524